-
Overview
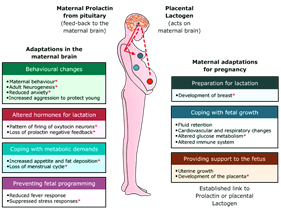 Noncancerous tumor (adenoma) of the pituitary gland in your brain is called prolactinoma. It overproduces the hormone prolactin which is called as hyperprolactinaemia. The major effect of increased prolactin is a decrease in levels of some sex hormones — estrogen in women and testosterone in men. Prolactinoma can impair your vision, cause infertility and produce other effects, although it isn’t life-threatening.
Noncancerous tumor (adenoma) of the pituitary gland in your brain is called prolactinoma. It overproduces the hormone prolactin which is called as hyperprolactinaemia. The major effect of increased prolactin is a decrease in levels of some sex hormones — estrogen in women and testosterone in men. Prolactinoma can impair your vision, cause infertility and produce other effects, although it isn’t life-threatening.Prolactinoma is one of several types of tumors that can develop in your pituitary gland.
Medications can often restore your prolactin level to normal and helping in treating prolactinoma. Surgery to remove the pituitary tumor also may be an option to treat prolactinoma.
-
Causes
These are tumors that develops in the pituitary gland. The cause of these tumors remains unknown.
A small bean-shaped gland situated at the base of your brain is called the pituitary gland. Despite its small size, the pituitary gland influences nearly every part of your body. Its hormones, such as prolactin, help regulate important functions such as growth, blood pressure and reproduction.
Prolactin overproduction can be due to medications, other types of pituitary tumors, an underactive thyroid gland, an injury to the chest, pregnancy and breast-feeding.
-
Symptoms
Increased level of prolactin in the blood can cause various symptoms. The symptoms differ slightly between men, women and children.
Symptoms in women may include:- Irregularity of periods or no periods.
- Reduction in fertility.
- Reduction in sex drive.
- Leaking of milk from the breasts (known as galactorrhoea). The milk may leak out by itself, or may only show when the breast is squeezed. (Note: leakage of milk from the breasts is normal towards the end of pregnancy, with recent childbirth, if breast-feeding, and for some time after finishing breast-feeding.)
- Rapid growth of hair on the face or body.
Symptoms in men may include:
- Reduction in fertility.
- Erectile dysfunction (difficulty having an erection).
- Decreased libido (reduced sex drive).
- Enlargement of breast (called gynaecomastia).
- Leakage of milk from the breasts.
Symptoms in children and teenagers may include:
- Decreased growth.
- Delay in puberty.
Large prolactinomas may press on the brain or nearby nerves (the nearest nerves are the optic nerves which go to the eye). This may cause symptoms such as:
- Headache.
- Symptoms with vision – you may get reduced vision or double vision. The early changes can easily go unnoticed, because they affect the peripheral vision – that is, the edges of your vision to the extreme left and right. This means that you may see less of what is around you, but can still see well if you focus on something directl
See a doctor urgently if you have headaches or reduced vision – you may need to have treatment promptly to relieve the pressure on the optic nerves. The prolactinoma, rarely, may press on the rest of the pituitary gland, stopping it from producing other hormones. This can cause symptoms such as tiredness, fainting, low blood pressure, low blood sugar or collapse. Also, rarely, there may be a leakage of the fluid that surrounds the brain and pituitary gland, felt as watery fluid leaking through the nose. These symptoms need urgent treatment.
-
Diagnosis
Symptoms can suggest diagnosis. Women tend to be diagnosed earlier than men, because a change in the woman’s periods is an early symptom and is easily noticed. Some prolactinomas are diagnosed by chance, if you have tests for another reason. If a prolactinoma is suspected, you may be offered several tests.
Blood tests
Level of prolactin can be checked in. If a high prolactin level is found, you may be asked to have a repeat test. This is because prolactin levels can be affected by many other things in the body, such as sleep or stress. It may help to take the blood sample when you are reasonably rested and have been awake for at least two hours.
Prolactin levels can range greatly and the normal level of prolactin is less than 400 mU/l. A very high prolactin level (>5000 mU/l) usually means that a prolactinoma is present. Levels in between may be due to a prolactinoma, or to other causes.
At the same time, other blood tests may be done. It is important to test the thyroid gland and to check kidney function, as both these can affect prolactin levels. Further tests may be needed to see if the tumour is causing a lack of other hormones made by the pituitary.
Eye tests
These tests will evaluate if the tumour is pressing on the optic nerve – this includes a test of visual fields.
>Scans
Size of the tumor can be evaluated by a magnetic resonance imaging (MRI) scan or a computed tomography (CT) scan. A bone density scan may be advised for some patients, to check whether you are at risk of osteoporosis (which is a possible complication – see below).
-
Complications
Prolactinoma can have complications which may include:
- Loss of vision. Left untreated, a prolactinoma may grow large enough to compress your optic nerve.
- Hypopituitarism. Pressure on the normal pituitary gland, with larger prolactinomas, can cause dysfunction of other hormones controlled by the pituitary, resulting in hypothyroidism, adrenal insufficiency and growth hormone deficiency.
- Loss of bone loss (osteoporosis). Too much prolactin can reduce production of the hormones estrogen and testosterone, resulting in decreased bone density and an increased risk of osteoporosis.
- Complications of pregnancy. During a normal pregnancy, a woman’s pituitary gland enlarges and prolactin production increases. A woman who has a large prolactinoma and becomes pregnant may experience additional pituitary growth and associated signs and symptoms, such as headaches and changes in vision.
Discuss the situation with your doctor if you have prolactinoma and you want to become or you already are pregnant. This is because adjustments in your treatment and monitoring may be necessary.
-
Treatments
Goals of treatment are:
- Reduce the production of prolactin to normal levels
- Normal pituitary gland function restoration
- Galactorrhea elimination
- Reduction in the size of the pituitary tumor
- Abolish any signs or symptoms from tumor pressure, such as headaches or vision problems
Treatment of prolactinoma consists of two main therapies, medications and surgery
Medications
Drugs given by mouth often can decrease the production of prolactin and eliminate symptoms. Medications may also shrink the tumor. However, long-term treatment with medications is generally necessary.
Known drugs such as dopamine agonists can be used to treat prolactinoma. These drugs mimic the effects of dopamine — the brain chemical that normally controls prolactin production — but are much more potent and long lasting. Commonly prescribed medications include bromocriptine (Cycloset, Parlodel) and cabergoline. These drugs decrease prolactin production and may shrink the tumor in most people with prolactinoma. During pregnancy, bromocriptine is the preferred drug when treating women who want to restore their fertility because its safety in pregnancy is well established. During pregnancy, your doctor will likely advise you to stop taking bromocriptine or carbergoline.
Doctors generally prefer to keep medications to a minimum while you’re pregnant, although these medications are considered safe in pregnancy. However, if you have a very large tumor, your doctor may recommend that you continue to take your medication during your pregnancy to prevent complications from the prolactinoma. If you’re being treated for prolactinoma and you’d like to start a family, it’s best to discuss your options with your doctor before you become pregnant.
The common side effects of these drugs are lightheadedness, nausea and nasal stuffiness are common side effects of these medications. However, these side effects often can be minimized if your doctor starts you with a very low dose of medication and gradually increases the dose. Cabergoline has less frequent and less severe side effects, but it’s more expensive than bromocriptine and newer, so its long-term safety record isn’t as well established. There have been rare cases of heart valve damage with cabergoline. Some people may also develop compulsive behaviors, such as gambling, while taking these medications.
You may be able to eventually stop taking the medication if medication effectively shrinks the tumor and your prolactin level remains normal for two years afterward,. Your doctor can offer you advice on when this may be possible for you. However, don’t stop taking either drug without your doctor’s approval.
Surgery
Surgery may be an option for the removal of a pituitary tumor if drug therapy for the treatment of prolactinoma doesn’t work or you can’t tolerate the medication. It may also be necessary to relieve pressure on the nerves that control your vision.
The size and extent of your tumor determines the type of surgery you require:
- Transsphenoidal surgery. This is the most common procedure. In this surgery, the tumor is removed through the nasal cavity. Complication rates from this type of surgery are low because no other areas of the brain are touched during surgery, and this surgery leaves no visible scars.
- Transcranial surgery. You may need a transcranial procedure, also known as a craniotomy, if your tumor is large or has spread to nearby brain tissue. This procedure involves accessing the tumor through the upper part of the skull.
Surgery outcomes largely depend on the size and location of the tumor and your prolactin levels before surgery. The higher the prolactin level, the slimmer the chance that your prolactin production will return to normal after surgery. Surgery corrects the prolactin level in most people with small pituitary tumors. However, many pituitary tumors come back within five years of surgery. For people with larger tumors that can only be partially removed, drug therapy often can return the prolactin level to a normal range after surgery.
External Links/References
http://www.mayoclinic.com/health/prolactinoma/DS00532
http://www.patient.co.uk/health/Prolactinoma.htm
http://women.webmd.com/amenorrhea-galactorrhea-syndrome

